 Causes can include lead displacement, lead fracture, exit block, myocardial infarction, and electrolyte abnormalities.įailure to sense : Failure to sense occurs when a pacemaker is not detecting or understanding intrinsic cardiac activity, resulting in asynchronous pacing (i.e pacer spikes within the cardiac cycle as shown below). This means that the pacer stimulation does not result in the expected myocardial depolarization. In the case of active dual chamber pacing, one would see pacer spikes before both the P wave and the QRS complex.įailure to capture : Pacer spikes without following P waves or QRS complexes is termed failure to capture. One can also see two pacer spikes before a narrow QRS in a biventricular pacemaker. If the pacer spike appears after the P wave but before a narrow QRS then biventricular pacing is likely. If the pacer spike is seen after an intrinstic P wave and before a wide QRS complex with left bundle branch pattern, the pacer is likely to be a single right ventricular pacing device (see below). In an atrial paced ECG, pacer spikes will appear before a normal morphology P wave (see below). Paced ECGs should be assessed systematically, similar to other ECGs, paying special attention to the location of the pacer spikes in relation to the P waves and the morphology of the QRS complex. If there is any intrinsic depolarization in either chamber, pacing will be inhibited in that chamber. Letter 3 – Sensing response: sensing response can be triggered, in which a depolarization results in a pacemaker discharging inhibited, in which depolarization inhibits pacemaker discharging dual, in which both inhibition or triggering can occur and none, in which neither triggering nor inhibition occursįor example, a common setting, DDD, signifies that both intrinsic atrial and ventricular activity are sensed and both atrial and ventricle are paced accordingly. Letter 2 – Chamber sensed: chamber where intrinsic depolarization is detected Letter 1 – Chamber paced: chamber where pacemakers leads are located 
For patients in the ED, it is important to focus on the first three letters: The North American Society of Pacing and Electrophysiology/British Pacing and Electrophysiology Group (NASPE/BPEG) Pacemaker code is a five-letter series that describes the settings of a patient’s pacemaker. How do we interpret this ECG? What are the significant findings that can discern information about the type of pacemaker placed?īefore discussing the ECG above, it is important to understand the basics of interpreting the ECG of a patient with a pacemaker. For patients with refractory Afib and reduced systolic function, the nodal ablation and pacemaker approach showed small but statistically significant improvement in echocardiographic parameters as well.įollowing placement of the pacemaker, the following ECG was obtained. One meta-analysis comparing AV-nodal ablation with pacemaker to pharmacologic therapy alone for refractory afib found that AV-nodal ablation/pacemaker led to a significant improvement in quality of life and symptoms with minimal morbidity. The European Society of Cardiology guidelines are similar but suggest first considering direct catheter-based or surgical ablation to eliminate the abnormally firing impulses in the atrium. According to American College of Cardiology/American Heart Association/Heart Rhythm Society guidelines, this is a reasonable approach when pharmacological therapy is inadequate and rhythm control cannot be achieved. Doing so, however, necessitates a pacemaker to generate a heart rate to provide appropriate cardiac output.  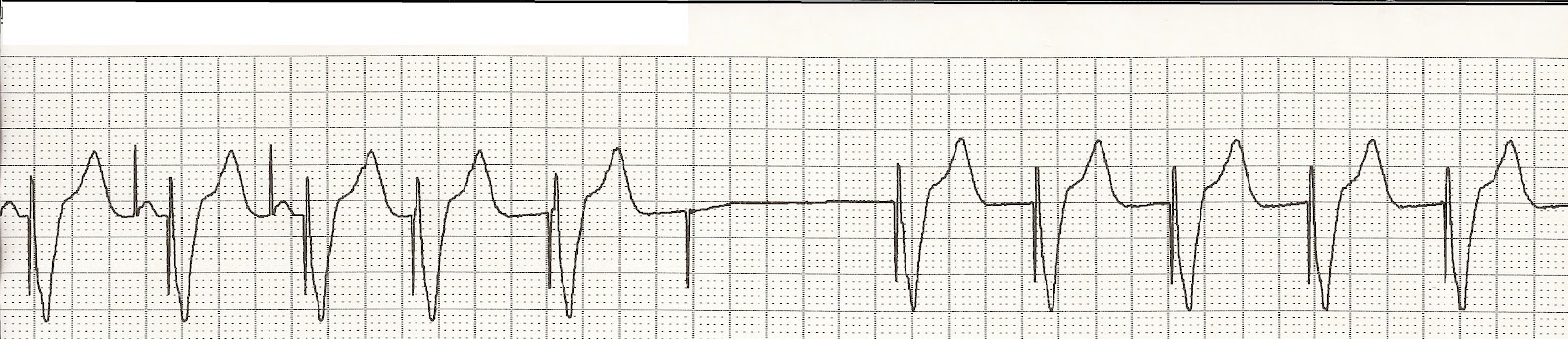
By ablating the AV node and blocking impulse conduction through it, the misfiring atrium is ignored. Ultimately, the patient underwent AV node ablation and dual chamber permanent pacemaker placement. Cardioversion was contraindicated as TEE demonstrated evidence of thrombosis in the left atrial appendage. The Afib with RVR remained uncontrolled despite high doses of esmolol and metoprolol. The patient was transferred to the CCU and started on an esmolol drip and metoprolol. However, over the course of one week, her Afib with RVR recurred and persisted with rates 130s-160s, not responding to nasogastric or IV medication. Initially, rate control was attempted with metoprolol via nasogastric tube. During the inpatient admission, the patient developed new-onset atrial fibrillation (Afib) with rapid ventricular response (RVR) (ECG below). 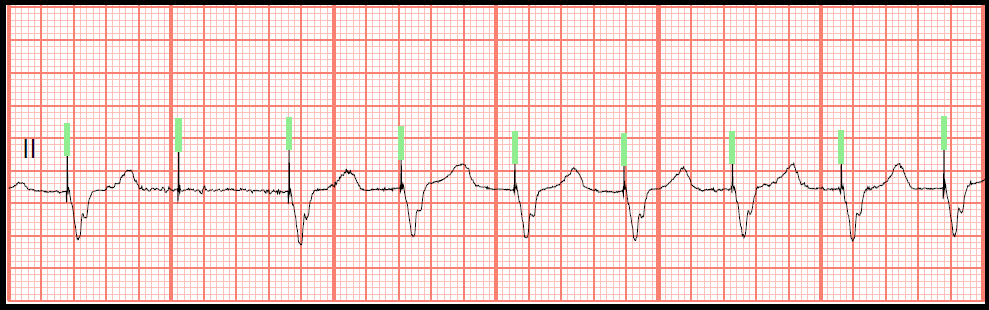
Peer Editors: Alec Feuerbach and Nicole AnthonyĪ 72-year-old female with a past medical history of hypertension, hyperlipidemia, asthma, CVA with residual right sided weakness and aphasia was admitted to the hospital from subacute rehabilitation after a recent subacute infarct. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
